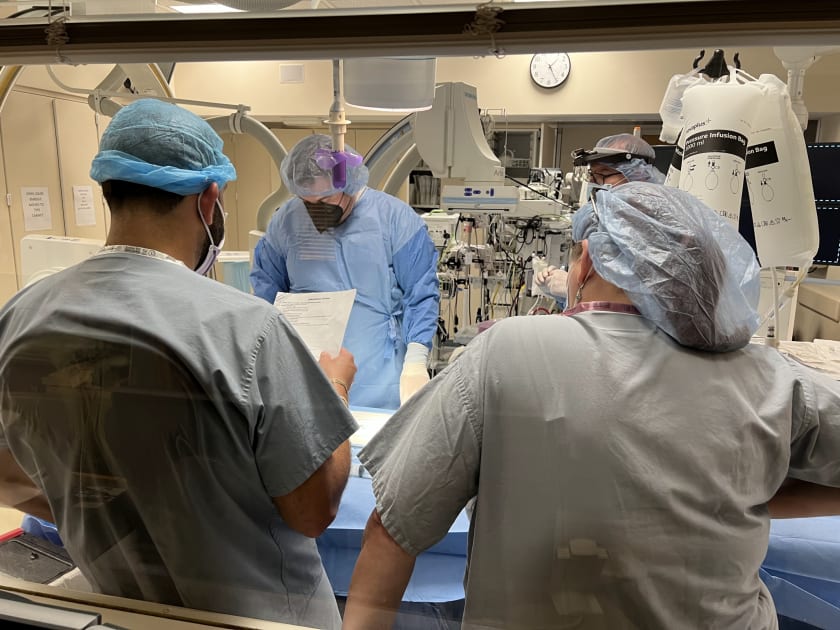
Yale Neurosurgeons Implant First Endovascular Device for Hydrocephalus in North America
A leading expert in neuroendovascular surgery, Charles Matouk, MD, and his team at Yale School of Medicine are now paving the way for better treatments for adult-onset hydrocephalus by being the first in the country to implant the eShunt device, an investigational device that can be placed using minimally invasive techniques.
Hydrocephalus is a common neurosurgical disease that causes cerebrospinal fluid (CSF) buildup in the brain. In adults, this can cause headaches, nausea and vomiting, gait disturbances, loss of balance, lethargy, impaired vision, memory loss, and mild dementia.
The most common current treatment, a ventriculoperitoneal (VP) shunt, leaves room for improvement. It requires a burr hole drilled into the skull and the implantation of long shunt tubing that extends from the brain to the abdomen, an invasive technique with frequent complications. In the scientific literature, 40% of cases lead to a complication or failure within one year; 50% of cases lead to complication or failure within two years.
Dr. Matouk, associate professor of neurosurgery at Yale School of Medicine and Chief, Neurovascular Surgery at Yale New Haven Hospital, leads the highest volume Normal Pressure Hydrocephalus (NPH) program in the state of Connecticut. The program provides dedicated staff and a systematic approach that more accurately predicts whether a patient will respond well to treatment or not.
High patient volumes and neuroendovascular expertise made Yale an ideal clinical site to study the eShunt device, says Dr. Matouk. The eShunt system, invented by neurosurgeons Carl Heilman, MD, and Adel Malek, MD, Ph.D., uses neuroendovascular techniques by traveling up blood vessels from the leg to get to the base of the skull. From there, the surgeon accesses a cistern – part of the brain that holds CSF – at the base of the skull using a needle with a miniature stent tucked inside. When the needle is withdrawn, the three centimeter stent is left behind, connecting the cistern to the bloodstream and allowing excess fluid to drain. This tiny shunt mitigates the need to drain brain CSF into the abdominal cavity using a long plastic tube tunneled under the skin.
Until recently, neurosurgeons have only used endovascular techniques to treat brain blood vessel conditions such as aneurysms or strokes. Those techniques have been tremendously successful in reducing patient complications and recovery time for things like aneurysms, arteriovenous malformations, stroke, and carotid stenosis. Now, surgeons are exploring ways they can access other parts of the brain using the blood vessels as “roads to get where you need to go,” says Dr. Matouk. Last year, a group of scientists at Mount Sinai was the first to endovascularly implant a brain-computer interface that helped patients translate their thoughts into digital output. The eShunt device is only the second example of an interventional device designed to treat a brain problem not involving the brain’s blood vessels.
Dr. Matouk, who completed his residency at the University of Toronto 12 years ago, says he is living in the future he envisioned from the beginning of his career.
“When I was a neurosurgery resident one of my mentors convinced me to train in neuroendovascular surgery not because he saw it as a way to treat blood vessel disorders, but he saw it as a way to access the brain without opening the skull. So, I always had that in mind from the very beginning,” says Dr. Matouk.
Since then, Dr. Matouk has seen the field of endovascular surgery mature. Technology has enabled device manufacturers to further miniaturize their products, which opens doors for surgeons to innovate.
“I’ve spent my career studying the roads to get to the brain and travel through it without opening the head and this is the first culmination of that vision to treat a common neurosurgical problem, hydrocephalus,” he says. “It’s so exciting 20 years later to be able to be involved in the first application of such a novel device.”